What is Sever’s Disease?
Sever’s disease is a prevalent condition resulting in heel pain among children and adolescents. Despite the potential intensity of pain, it’s a self-limiting issue that usually doesn’t lead to long-term complications. It’s notably the primary reason for heel pain in young children and adolescents.
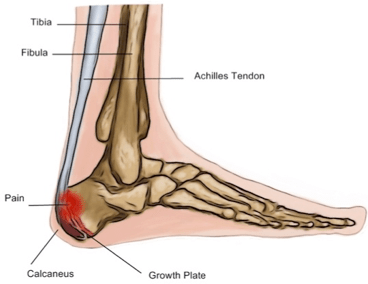
Termed as calcaneal apophysitis, it’s an inflammation of the heel’s growth plate, which is a bone section responsible for growth in an expanding skeleton and can be more fragile than other bone regions. This area, when subjected to excessive or repetitive stress, can become inflamed and painful.
What are the symptoms?
Youngsters might report heel pain that escalates during activities like walking, running, or jumping. This can manifest after heightened physical activity or post a growth spurt. The pain might also be noticeable while walking on heels.
Why does this happen?
The Achilles tendon, connecting to the heel’s rear adjacent to the growth plate, exerts force during walking. If this force exceeds a limit, the growth plate might get irritated, triggering a painful inflammation.
Though heightened activity can be a significant contributor, other factors might play a role, such as limited ankle mobility, abnormal foot movements during walking, or tight calf muscles. There are instances when Sever’s disease might arise without any evident trigger.
What is the treatment?
While Sever’s disease is self-limiting and generally resolves once growth is complete, it can be painful, potentially influencing a child’s activity regime and walking pattern. To counteract any long-term complications due to alterations or inactivity, physiotherapists can guide your child towards maintaining optimal movement with minimal pain. Common solutions include patient education, rest, or discontinuation of activities causing pain. Recent research suggests that custom orthotics can mitigate pain while preserving activity levels. Physiotherapy can tackle underlying causes, such as unusually tight muscles or poor walking patterns, and offer pain relief strategies or recommend alternative exercise modes if required. For comprehensive details, consult your physiotherapist.
Note: The content in this article is not a substitute for professional medical advice. Always consult a medical expert for individualized guidance.



